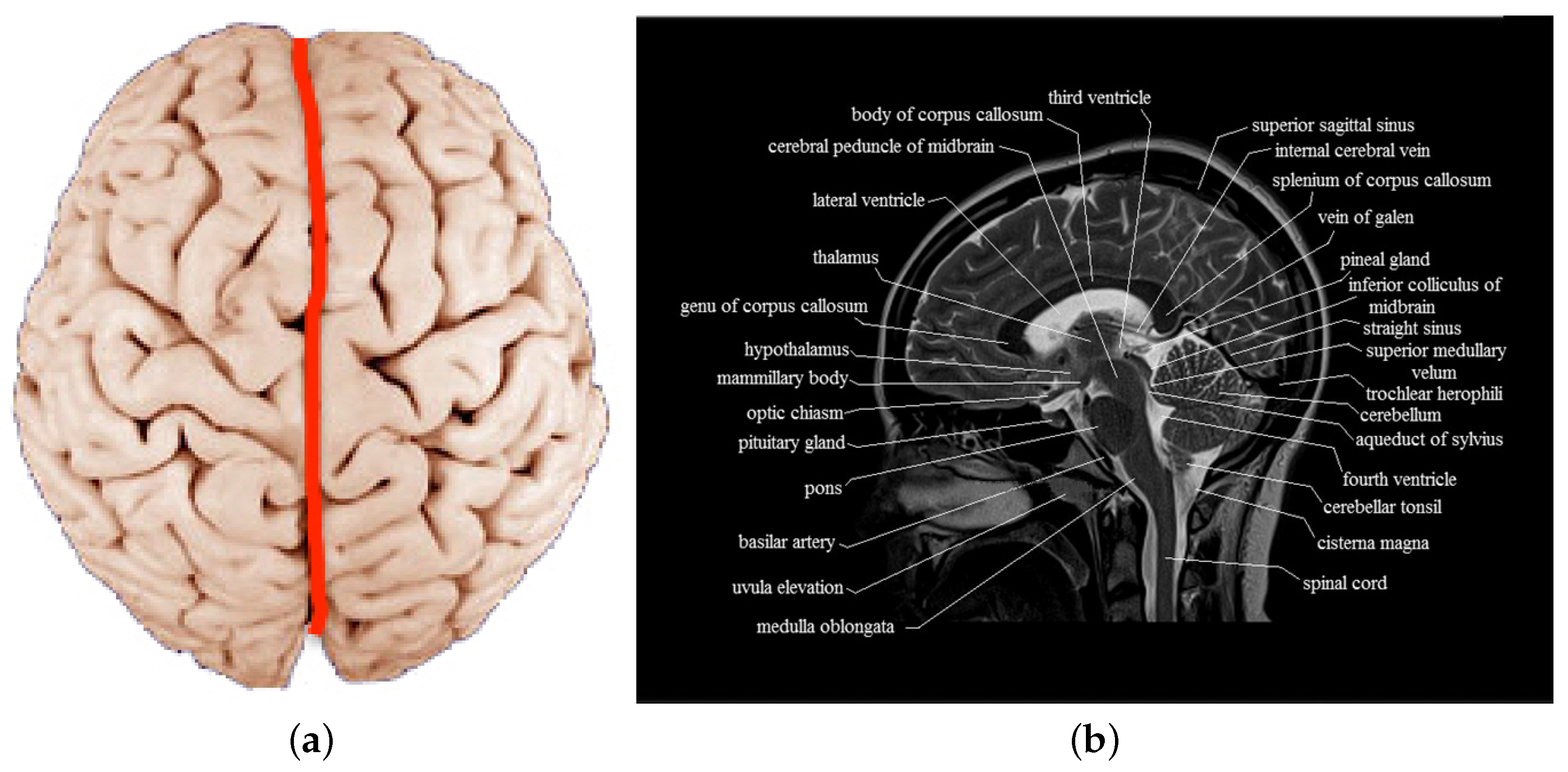
This cluster, labelled as ‘intralesional’, is no longer evident in the postoperative fMRI study due to the removal of the dysplastic area. In the presurgical examinations (A, D), the cluster of BOLD pixels located inside the lesion (white arrows from A and D to C) correctly correlates with the fMRI paradigm. The red line indicates the GLM model of HRF response and the black one the raw signal registered during the acquisition). The time course of the BOLD signal of the area indicated in the preoperative images is showed in C (red line, time course of the task black line, the variation of the BOLD signal during the task. Structural MRI shows a left frontal malformed area located on a irregularly flat gyrus whose subcortical white matter is mostly hyperintense. BOLD functional correlated signals (red-yellow colormap) are superimposed on axial FLAIR images (A, presurgical B, postsurgical) and sagittal FLAIR sections (D, presurgical E, postsurgical) across the lesion and the surgical breach (see white vertical lines). Right-handed 15-year-old girl with left frontal FCD IIb and left dominance for language.

Focal lesional epilepsy associated with diffuse EEG abnormalities may favor atypical language lateralization and worse cognitive performances, which are potentially reversible after successful surgery. Neither preoperative asymmetry nor postoperative DTI LI changes in the arcuate fasciculus were observed. Abnormal postoperative EEG (p = 0.003) and surgical failures (p = 0.015) were associated with more atypical language lateralization, in turn correlating with worsened fluency. Postoperative language reorganization implied shifting towards atypical language representation. Diffuse interictal EEG abnormalities predicted a more atypical language representation on fMRI (p = 0.012), which in turn correlated with lower attention (p = 0.036) and IQ/GDQ scores (p = 0.014). Preoperatively, we found atypical language lateralization in four patients during WG task, in one patient during RG task and in seven patients during the comprehension task. We analyzed possible changes of fMRI and DTI LIs and their clinical predictors. Twenty out of 29 patients also underwent postoperative language fMRI. We first assessed patterns of language representation (relationship of activations with the epileptogenic lesion and Laterality Index (LI)) and then hypothesized a causal model to test whether selected clinical variables would influence the patterns of language representation and the ensuing impact of the latter on cognitive performances. We also acquired DTI data on arcuate fasciculus in 24 patients.
All patients were consecutively enrolled at a single epilepsy surgery center between 20 and assessed with preoperative structural and functional 3T brain MRI during three language tasks: Word Generation (WG), Rhyme Generation (RG) and a comprehension task. In 20 of them, we also assessed the influence of epilepsy surgery on language lateralization. In this prospective study, we used fMRI and DTI to explore patterns of language representation, their predictors and impact on cognitive performances in 29 children and young adults (mean age at surgery: 14.6 ± 4.5 years) with focal lesional epilepsy.

In fact, most of the evidence on this topic derives from cross-sectional or retrospective studies in adults submitted to anterior temporal lobectomy. However, presurgical language mapping using either functional or structural networks can be challenging, especially in children. Mapping brain functions is crucial for neurosurgical planning in patients with drug-resistant seizures.
